6 June 2019
Our own Joseph Casey, Deputy Director of Programme Delivery at King’s Health Partners, blogs about all things Vital 5 and how the programme is expected to impact people’s health outcomes for the better.
At the King’s Health Partners annual conference last month, Prof John Moxham shared the work we are undertaking with others across south east London to develop the Vital 5. This blog accompanies John’s presentation, which is available on our website.
Together, we face significant challenges to future health and wellbeing, alongside major and on-going sustainability challenges for health and care services. We know that across the United Kingdom life expectancy is stalling, health inequalities are growing, and that these trends are affecting us to a greater degree than many other developed economies.
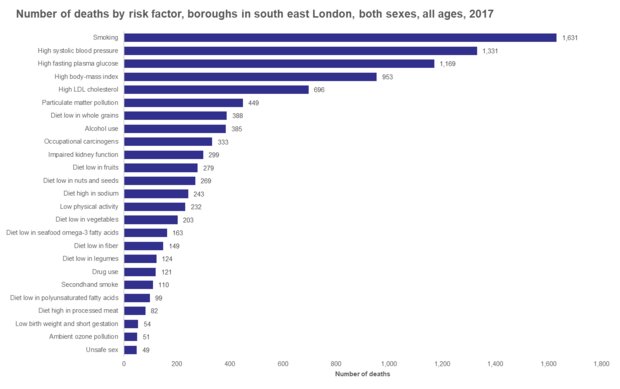
We also know that poor health comes from somewhere. The Global Burden of Disease investigates the mortality and morbidity from major diseases, injuries and risk factors to health at global, national and regional levels. For the six boroughs of south east London, tobacco and high blood pressure remain the two major risk factors for diseases leading to death, and high body-mass index and alcohol use have both increased substantially since 1990.
[Image: The graph shows smoking to be the highest risk factor of death, followed by high blood pressure. Click the graph to see a full PDF]
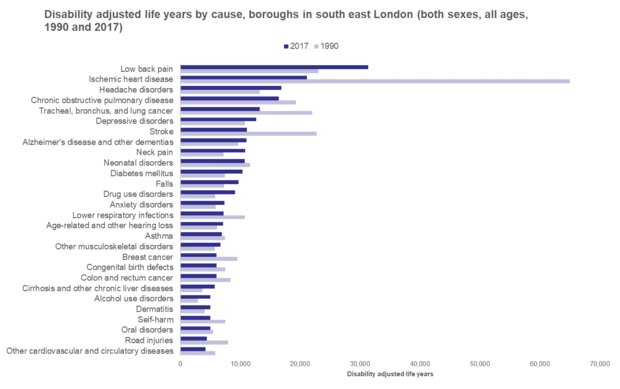
For the United Kingdom as a whole, 40% of disability adjusted life years lost are attributable to smoking, alcohol consumption, hypertension and obesity. Over the last thirty years, better detection and control of hypertension has had a substantial impact on the burden of disease (as shown below for south east London for conditions such as ischemic heart disease and stroke).
[Image: Analysis of data for Bexley, Bromley, Greenwich, Lambeth, Lewisham, and Southwark extracted from Institute of Health Metrics and Evaluation (online): https://
However, we know locally from research undertaken within King’s Health Partners that blood pressure is only well controlled for a quarter of the population with hypertension. Common mental health conditions – such as depression and anxiety – are increasing, and research commissioned by our partners at the Guy’s and St Thomas’ Charity shows that depression is the most common long term condition affecting younger people.
Together, these risk factor and conditions form the Vital 5:
- High blood pressure
- Obesity
- Alcohol
- Smoking status
- Mental health conditions
The aim of the Vital 5 is to improve population health and reduce health inequalities. To realise this vision, we are working with people from a range of backgrounds and organisations to develop and implement the Vital 5.
In her annual report, the Chief Medical Officer for England argued that “maintaining ‘good health’ and preventing ‘ill-health’ is an investment for the future. This is so important that we need to measure and track health in our society”. Our aim is that the routine recording and reporting of the Vital 5 – and the health actions put in place to respond to it – will substantially increase value across the health and care system by promoting a sense of shared ownership and responsibility for local people and professionals alike.
This will be supported through system-wide collection for whole population analysis, supporting all those involved in improving health and wellbeing to make decisions together and understand the impact and outcomes.
We are working and talking with as many different people as we can. To support this, we will shortly be launching a series of conversations to bring people together locally to share experience and expertise. We would really like to hear from people who want to be involved, please contact kingshealthpartners
Read more about the Vital 5 and Value Based Healthcare on the King's Health Partners website.